To Our Valued Provider Partners:
We are writing to inform you of upcoming administrative changes that will affect your patients who are MedCost Benefit Services members.
In July 2025, MedCost LLC was acquired by Health Plans, Inc. (HPI), a national third-party administrator (TPA) based in Westborough, Massachusetts. MedCost LLC consists of MedCost’s proprietary networks and its third-party administrator (TPA), MedCost Benefit Services. Throughout 2026, MedCost Benefit Services will transition existing clients to HPI’s claims administration system using a phased approach.
The first phase will take effect on May 18, 2026, with additional phases planned for July and October.
What This Means For You
Importantly, your participation in the MedCost Network (or MedCost Virginia Network, if applicable) remains unchanged. You will continue to see these members as you do today, and your contracted network status is not impacted.
What Will Change
As MedCost Benefit Services employer groups transition to HPI, you may notice the following administrative updates:
ID Cards
- Members will begin presenting new HPI medical/pharmacy ID cards that include:
- HPI’s logo, along with the employer’s logo and the appropriate MedCost network logo. (See sample below.)
- New HPI group and member ID numbers.
- Updated Customer Service and precertification contact information.
- Once a MedCost Benefit Services employer group has transitioned to HPI, all inquiries (including those for dates of service prior to transition) should be directed to HPI Customer Service, using the number on the member’s ID card.

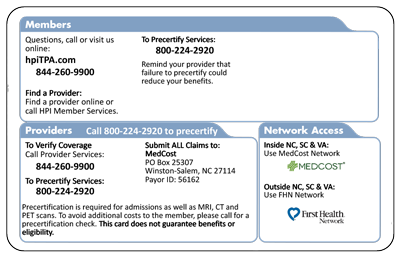
Members have been advised to present their new ID cards to providers and pharmacies at their first visit on or after the effective transition date.
Provider Portal Access
- For members presenting an HPI ID card, please use the HPI provider portal at hpitpa.com to access:
- Eligibility and benefits information
- Claims payment status
- Continue using the MedCost Benefit Services provider portal to access information for members who have not yet transitioned to HPI.
Communications
- You may begin to see HPI’s name on administrative communications, such as Explanation of Benefits (EOBs).
What Will Stay the Same
- Your MedCost (or MedCost Virginia) network participation remains unchanged.
- As a participating MedCost network provider, you will continue to use MedCost provider web application services for:
- Claims Submission and Repricing
- Provider Reference Guide
- Claims submission remains the same:
- Continue using the same EDI for electronic claims.
- Continue using the same mailing address for paper claims.
Remember to include the new HPI Group Number and HPI Member ID (if applicable) when filing claims.
- Existing precertifications and prior authorizations remain in effect.
- Member benefits will not significantly change.
- Member cost shares (copays, coinsurance, deductibles) remain the same.
Our Commitment
We are working to ensure a smooth transition with minimal disruption to your practice. These changes are administrative in nature and are designed to support improved long-term capabilities.
If you have questions, please refer to the customer service number on the member’s ID card or contact MedCost Network Services at [email protected].
Thank you for your continued partnership and the care you provide to our members.
Sincerely,
MedCost in partnership with Health Plans Inc. (HPI)
